Phentermine Side Effects
This article is for informational purposes only and should not be used as a substitute for professional medical advice. Always consult your healthcare provider before starting any new medication or supplement regimen.
Phentermine commonly causes side effects like dry mouth, insomnia, increased heart rate, and changes in taste. Serious but rare risks include pulmonary hypertension, heart valve disease, and psychological dependence.
Too busy for the full read? Here’s what you need to know:
Common Side Effects of Phentermine
The most commonly reported phentermine side effects by patients include (
Each of these side effects should be closely monitored, and if they persist or worsen, a healthcare provider should be consulted. It’s also important for users to understand that while these side effects are common, they are not experienced by everyone and can vary in intensity.
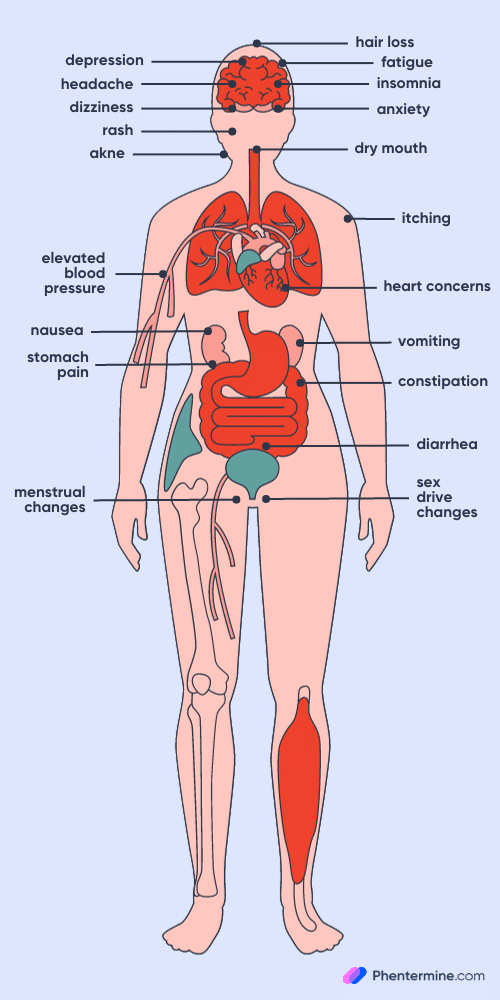
According to a recent online poll conducted by phentermine.com with over 2100 phentermine users (
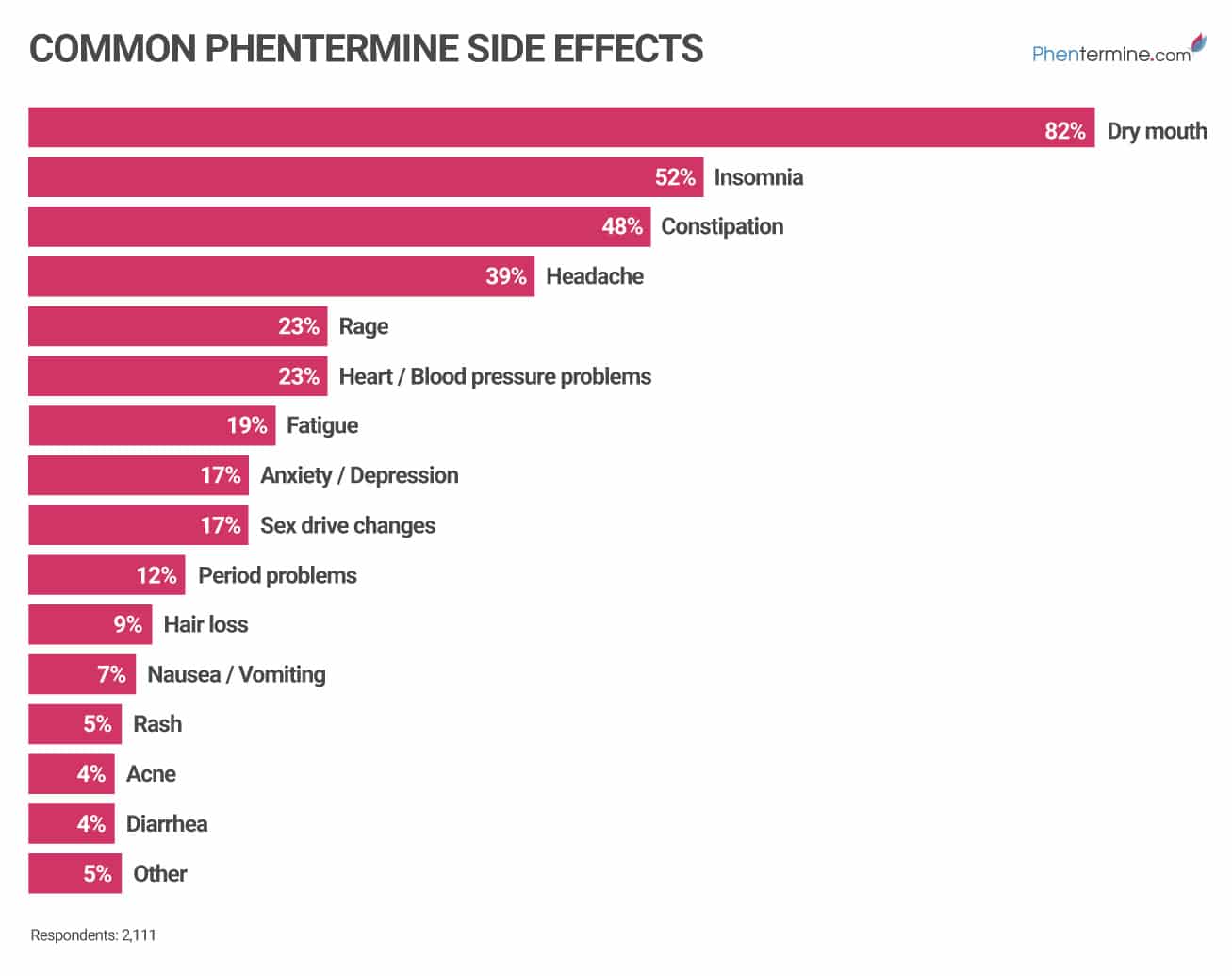
These findings are confirmed by a study published in the Expert Opin Drug Saf. by Derosa & Maffioli (
Serious Side Effects and Risks
When used as prescribed, Phentermine can be an effective weight loss tool. However, it’s not without its risks, especially when taken over long periods or misused. Below are some of the serious side effects and risks associated with phentermine:
The rare reports of both Primary pulmonary hypertension (PPH) and valvular heart disease were primarily observed in a group of patients that took the once-popular combination of phentermine and fenfluramine (colloquially referred to as “phen-fen”) in the mid-1990s (
Symptoms of severe phentermine side effects include (
- Chest pressure or pain
- Pounding or irregular heartbeat, or fluttering in your chest
- Lightheadedness or faintness
- Dizziness or fainting spells
- Shortness of breath, even with only mild exertion
- Swelling in your legs, ankles, or feet (edema)
- Slurred speech or weakness on one side of your body
- Blue lips and skin
- Rapid pulse or pounding heartbeat
- Unusual thoughts or behavior, such as confusion, irritability, phen rage, or hallucinations
- Extreme happiness or sadness (euphoria or phentermine depression)
- Any indicators of dangerously high blood pressure, such as severe headache, blurred vision, buzzing in your ears, anxiety, confusion, chest pain, shortness of breath, uneven heartbeats, or seizure.
Call 911 (emergency medical services) or go to a hospital right away if you notice any of these symptoms while taking phentermine.
It’s imperative for users to be aware of these risks and to use phentermine only under the guidance of a healthcare professional. Long-term use should be approached with caution, and any decision to extend use beyond the recommended duration should involve a thorough risk-benefit analysis by a healthcare provider.
Phentermine Side Effects in Females
Phentermine can cause several concerning side effects specific to women.
- Menstrual Irregularities: Phentermine doesn’t directly impact hormone levels; however, women’s hormones are sensitive to nutrient scarcity or stress. An insufficient caloric intake or elevated stress levels can cause hormone fluctuations, affecting menstrual cycles. The menstrual cycle can be disrupted, irregular, or absent (
25 ). Birth control or hormone replacement therapy may ease this effect. - Changes in libido: Phentermine can affect sexual desire. In men, it can cause erectile dysfunction. In women, it can change libido and cause discomfort during sex (
10 ). - Contraindication in Pregnancy: Phentermine is unsafe during pregnancy. While using phentermine may indirectly improve fertility in overweight or obese individuals, it is important to use contraception to prevent pregnancy while taking the drug. If planning to conceive, discontinue the use of phentermine. Limited research exists on the effects of phentermine on birth defects or miscarriages during pregnancy. Although a small study (
26 ) found no higher rate of miscarriages in first-trimester users, insufficient data makes it difficult to determine if phentermine crosses the placenta. - Contraindication for Breastfeeding Mothers: Due to safety concerns for the baby, there is limited research on the effects of phentermine on breastfeeding mothers. Therefore, it is not advisable for breastfeeding mothers to use phentermine as it can potentially harm the baby through breast milk. If you are a breastfeeding mother seeking assistance with weight loss, it is recommended to consult your healthcare provider. Regular exercise and a healthy diet are the safest approaches to weight loss during breastfeeding. Phentermine typically takes 3 to 5 days to exit your system completely.
- Impact on Postmenopausal Women: Weight gain is common among postmenopausal women, with around 20% experiencing a significant increase. Factors like aging and reduced energy contribute to this, but menopause and hormonal changes specifically lead to abdominal fat accumulation. However, addressing obesity is important for cardiovascular health. Losing 5% to 10% of body weight can bring significant benefits, and healthcare providers may suggest dietary changes and exercise before considering medications like phentermine. When prescribing weight loss medication, caution is necessary for menopausal women, especially those with heart conditions.
Phentermine Side Effects In Males
Men may experience certain side effects when taking phentermine, including alterations in sexual desire or performance, such as a decrease in libido or erectile dysfunction (
As with all users, additionally, phentermine commonly causes an elevated heart rate, increased blood pressure, and feelings of nervousness.
It should be noted that these side effects can vary from person to person, and not everyone will encounter them. Before initiating any medication, it is crucial to consult with a healthcare professional to discuss potential side effects and determine the suitability of phentermine for individual circumstances.
How Soon Do Side Effects Start?
The most common side effects of phentermine can occur shortly after taking the first dose. These include dry mouth, insomnia, dizziness, constipation, and increased heart rate and blood pressure. These symptoms are usually mild and tend to diminish as the body adapts within the first couple of weeks.
More serious but less common side effects may emerge with prolonged use. These include pulmonary hypertension, valvular heart disease, dependence and addiction, and psychosis. These side effects are closely associated with long-term use of phentermine beyond a few weeks or months.
Withdrawal side effects can occur within 12-24 hours after stopping phentermine. Symptoms include depression, fatigue, disturbed sleep patterns, and increased appetite. Withdrawal can be minimized by tapering off phentermine slowly under medical supervision.
Individual responses to phentermine vary based on age, health, concurrent medications, and lifestyle. Certain groups may experience side effects sooner or more severely, including the elderly, those taking high doses, and those with pre-existing medical conditions like diabetes, thyroid disorder, or glaucoma.
How Long Do Side Effects Last?
Common side effects such as headaches, dizziness, nausea, and insomnia typically diminish within 1-2 weeks as the body adapts to the medication. As tolerance develops, these symptoms often resolve.
Desirable effects like increased energy and appetite suppression may last longer, aligning with the drug’s ongoing activity in the body.
More serious side effects like chest pain would require immediate medical attention. But most milder issues, assuming they are not severe or intolerable, can be expected to subside within 10 days to 2 weeks tops as the body accommodates to the stimulant properties of phentermine.
What Are the Long-Term Side Effects?
The long-term use of phentermine can lead to several serious side effects as the drug is FDA-approved for short-term use, which means for no more than 12 weeks at a time:
- Cardiovascular effects: Phentermine can raise blood pressure and heart rate. With long-term use, this may increase the risk of heart disease, heart attack, stroke, and other cardiovascular complications.
- Pulmonary hypertension: Rare but potentially fatal cases of pulmonary arterial hypertension have been linked to long-term use.
- Heart valve damage: Extended use (over 3 months) can cause heart valve defects like leaky mitral and aortic valves. This may require valve replacement surgery.
- Dependence and addiction: Long-term use can lead to psychological and physical dependence, addiction, difficulty in stopping the medication, and withdrawal symptoms.
- Tolerance: Over time, the body may become tolerant to phentermine, requiring higher doses to achieve the same effects. This increases the risks of toxicity.
- Neuropsychiatric effects: Extended use has been associated with anxiety, depression, psychosis, mania, suicidal thoughts, and other mental health issues.
- Nutritional deficiencies: Strong appetite suppression over months or years can result in severe nutritional deficiencies.
- Rebound weight gain: Discontinuing phentermine after prolonged use may result in rapid and excessive weight gain.
For these reasons, phentermine is only recommended for short-term use of up to 12 weeks. Careful medical monitoring is crucial if continued beyond this duration. The risks tend to outweigh any benefits with long-term therapy.
It has to be mentioned, however, that there is very little research on the long-term side effects of phentermine (
Managing and Treating Side Effects
If side effects do occur during Phentermine treatment, there are some steps you can take to help manage symptoms until tolerance builds:
- Stay hydrated: Drink plenty of water to stay hydrated. Dehydration can alleviate dizziness, headaches, and nausea.
- Eat regularly: Eat small, low-fat snacks or meals throughout the day rather than a few large ones. This can help stabilize energy levels and digestion.
- Over-the-counter remedies: Try over-the-counter antacids, Dramamine, or ginger capsules to counteract nausea, dizziness, or upset stomach.
- Dry mouth solutions: Use a humidifier, drink tea, suck on hard candy, or use Biotene mouthwash to soothe a dry mouth.
- Improve sleep: Practice relaxation techniques, limit screen time before bed, or try natural sleep aids like melatonin to promote better rest and combat insomnia.
- Check for interactions: Check that no other medications could be interacting to worsen side effects, and ask your doctor for guidance on that.
Seek medical attention if side effects are severe, intolerable, or persist beyond a few weeks. Contact your healthcare provider if you experience:
- Chest pain, palpitations, pounding heart, or difficulty breathing
- Blurry or double vision, dizziness when standing, or severe headaches
- Diarrhea, nausea/vomiting, or abdominal pain lasting more than a day
- Insomnia that impairs daily function despite remedies
- New or worsened mental health symptoms like anxiety or depression
- Any other concerning changes in your health status
With appropriate management and medical supervision, mild side effects are typically temporary. Always reach out for professional support if needed.
Contraindications and Precautions
Phentermine is contraindicated in certain medical conditions due to health concerns and an increased risk of side effects:
- Uncontrolled hypertension: Phentermine can raise blood pressure.
- Heart disease: This includes arrhythmias, coronary artery disease, congestive heart failure, history of stroke or heart attack. Stimulants can exacerbate these issues.
- Substance abuse: Including alcohol abuse. Stimulants may increase cravings or the risk of relapse.
- Glaucoma: Phentermine may increase eye pressure.
- Hyperthyroidism: Especially if uncontrolled.
- Pregnancy or breastfeeding: Safety for these groups is not established.
Extra caution is needed for those with diabetes, kidney or liver disease, mental health conditions (like anxiety or depression), or those taking medications such as MAOIs, insulin, or blood pressure drugs. These conditions may increase side effects or require dosage adjustments.
It’s critical to disclose your full medical history and all medications or supplements to your doctor before starting phentermine. Regular health monitoring and treatment response checks are important to ensure the safety and effectiveness of phentermine. Always consult a healthcare provider for proper screening and management.
Drug Interactions May Worsen Side Effects
As a stimulant medication, phentermine carries the risk of interacting adversely with certain other drugs and substances.
It’s crucial that your doctor knows about everything you’re taking so they can screen for interactions that may worsen side effects, reduce phentermine’s effectiveness, or endanger your health and safety.
Key interactions include:
- MAO Inhibitors (MAOIs): These antidepressants can dangerously increase blood pressure when combined with Phentermine. Avoid MAOIs for 2 weeks before and after Phentermine treatment.
- Insulin and oral diabetes medications: Dosages may need adjustment to prevent low blood sugar.
- Blood pressure medications: Close monitoring and possible dosage adjustments are necessary due to phentermine’s effects on blood pressure.
- Norepinephrine-Dopamine Reuptake Inhibitors (NDRIs): Drugs like bupropion may increase the risk of elevated blood pressure and heart rate when used with phentermine.
- Serotonergic drugs: Medications affecting serotonin (e.g., triptans for migraines) can lead to serotonin syndrome, a rare but serious side effect.
- Alcohol: Best avoided, as it can compound sedative effects and increase health/safety risks like dehydration.
- Illicit drugs: Combining phentermine with drugs like cocaine or methamphetamines can cause dangerous physiological reactions and side effects.
Always let your doctor know about everything you consume to ensure safe, appropriate care. Proper medical oversight ensures that phentermine is used responsibly and effectively for weight loss.
How to Avoid Phentermine Side Effects
Each phentermine side effect is treated differently depending on the reaction’s timing, severity, and nature.
However, here are a few common suggestions to manage phentermine side effects effectively:
- Lowest effective dose: Starting at the lowest approved dose and increasing slowly under medical guidance can help your body adjust gradually.
- Healthy lifestyle: Make healthy lifestyle changes like increasing activity, getting quality sleep, limiting alcohol/caffeine, hydrating, and eating balanced small meals throughout the day. This supports your overall well-being while taking phentermine.
- Full disclosure: Fully disclose all other medications and supplements to your doctor.
- Monitor symptoms: Monitor yourself for new or worsening symptoms and report concerns promptly so any needed adjustments can be made. Don’t wait until side effects become severe.
- Reminders: Consider setting reminders on your phone or calendar to take Phentermine with food if your dose requires it, as an empty stomach may exacerbate issues for some.
- Identify triggers: Try eliminating potential triggers one at a time, like spicy foods or artificial sweeteners, if you suspect they may aggravate symptoms in your case.
- Explore additional strategies: Inquire about other strategies your doctor recommends, like supplements or natural remedies to help counteract potential issues.
- Regular check-ups: Check in regularly with your prescribing practitioner, even if tolerating the medication well, to ensure it continues providing benefits safely over the recommended short-term timeframe.
Slow and careful approach, lifestyle adjustments, open communication with your healthcare provider, and attentive self-monitoring can help minimize phentermine side effects. Your safety and health are the top priorities.
When to Consult a Healthcare Provider
Before starting phentermine, obtaining a thorough medical evaluation by your primary care doctor or a weight management specialist is essential. This includes reviewing your health history, assessing contraindications, conducting necessary tests, and determining the suitability of phentermine for your care plan.
During your phentermine treatment:
While on Phentermine, be sure to attend all scheduled appointments and follow any instructions for ongoing testing and monitoring to ensure safe and effective treatment.
It’s also important to contact your healthcare provider promptly if you experience any concerning side effects, changes in your health or mood, difficulties adhering to the recommended treatment plan, issues managing side effects at home, or any questions regarding your care and progress.
Specifically, seek immediate medical attention for symptoms like persistent chest pain, palpitations, severe headaches, dizziness, difficulty breathing, severe abdominal pain, blurred vision, confusion, anxiety, or behavioral changes. Early identification and response to potential issues is key.
Overall, closely collaborate with your doctor to safely integrate phentermine into a personalized, healthy lifestyle plan. This approach aims for valuable short-term results under professional guidance, prioritizing your safety and long-term wellness.
Latest Research and Studies
Some recent research on phentermine’s side effects and safety considerations:
- A 2023 study in the South African Medical Journal concludes that patients receiving long-term phentermine therapy are at risk of experiencing moderate to severe drug-drug interactions, leading to serious adverse drug reactions. This raises concerns about the safety of long-term phentermine use and the need for careful consideration of potential drug interactions in such treatments (
14 ). - A 2022 paper in Cureus concludes that clinicians should be aware of cardiovascular side effects, especially the risk of coronary vasospasm in patients presenting with evidence of myocardial infarction without obstructive coronary artery disease. The paper emphasizes the importance of a detailed medical history, including medications and predisposing conditions, to help identify and possibly prevent exacerbation of such cardiovascular side effects (
15 ). - A 2019 study in Obesity examined overall weight loss and cardiovascular risk associated with longer-term phentermine use. It found no significant correlation between longer-term phentermine use and adverse cardiovascular outcomes (
16 ). - A 2019 case report in Clinical Psychopharmacology and Neuroscience discusses the need for caution in prescribing phentermine, especially considering its potential to cause recurrent psychotic episodes. It also underscores the importance of physicians being aware of the psychiatric side effects of phentermine and educating patients about these risks (
17 ). - A 2015 study in the Journal of Obesity & Metabolic Syndrome addresses common adverse events and serious side effects of anti-obesity drugs, including phentermine/topiramate that need monitoring, such as metabolic acidosis, urolithiasis, acute angle closure glaucoma, and teratogenic effects (
18 ). - A 2014 meta-analysis in the Journal of Hypertension examined cardiovascular data associated with long-term use of phentermine and topiramate extended-release (Qsymia). Findings indicate that this combination may be a safe and effective option for reducing weight in overweight/obese patients at low-to-intermediate cardiovascular risk (
19 ). - A 2012 paper in Expert Opinion Drug Safety concludes that phentermine is associated with side effects like dry mouth and insomnia. It further highlights that these side effects are generally mild to moderate and tend to decrease over time. Phentermine’s contraindications include a history of cardiovascular or psychiatric disorders, and it should not be combined with other centrally acting anorectic agents (
20 ). - A 2011 report published in The Texas Heart Institute Journal discusses the association of fen-phen use with valvular abnormalities, regurgitation, and PH, noting that withdrawal from the drug can lead to improvement in about half of the patients with mitral and aortic valve regurgitation (
21 ). - A 2011 review in CNS Neuroscience & Therapeutics reports adverse effects following phentermine treatment, including psychotic episodes, mania, and a sporadic incidence of depression and irritability in clinical studies. The review highlights that, however, these adverse effects are not described as widespread or consistently observed in all users of the drug (
22 ). - A 2010 study in Diabetes Obesity Metabolism reports dry mouth and insomnia as the most common adverse events. The study also noted that while no clinically severe adverse events were reported, phentermine, being a sympathomimetic amine, could potentially lead to side effects like insomnia, palpitation, the elevation of blood pressure, and gastrointestinal problems (
23 ). - A 2010 case report from the Yonsei Med Journal highlights that while drugs like phentermine (have been considered relatively safe for obesity treatment, certain cases suggest a potential link between phentermine and pulmonary hypertension (
24 ). - A 2002 systematic review in BMC Clinical Pharmacology in 2002 found that the risk of valvular heart disease was significantly increased by appetite suppressants, such as phentermine. It highlighted, however, that the overall risk is lower than earlier studies had indicated (
25 ).
Conclusion
Phentermine commonly causes side effects like dry mouth, insomnia, increased heart rate, and changes in taste or sexual function. Serious but rare risks include pulmonary hypertension, heart valve disease, and psychological dependence.
Using phentermine under medical supervision is crucial, as it’s intended for short-term use. Side effects can often be managed with lifestyle adjustments and medical guidance.
Long-term use increases the risk of serious health issues and should be carefully monitored by healthcare professionals.
- Rueda-Clausen, C.F., Padwal, R.S., Sharma, A.M. (2013). New pharmacological approaches for obesity management. Nature Reviews Endocrinology, 9(8):467-478.
- Velazquez, A. & Apovian, C.M. (2018). Updates on obesity pharmacotherapy. Annals of the New York Academy of Sciences, 1411(1):106-11.
- Kim KK, Cho HJ, Kang HC, Youn BB, Lee KR. (2006). Effects on weight reduction and safety of short-term phentermine administration in Korean obese people. Yonsei Medical Journal, 47(5):614-625. doi: 10.3349/ymj.2006.47.5.614
- Alexander, J., Cheng Y.H., Choudhary, J., Dinesh, A. (2011). Phentermine (Duromine) precipitated psychosis. Australian and New Zealand Journal of Psychiatry, 45(8):684-685.
- Members of “Losing Weight with Phentermine” Support Group on Facebook & Phentermine.com Forum. (2019, March 13). [User Report of Common Phentermine Side Effects]. Unpublished raw data.
- Derosa, G., & Maffioli, P. (2012). Anti-obesity drugs: A review about their effects and their safety. Expert Opinion on Drug Safety, 11(3), 459-471. doi:10.1517/14740338.2012.675326
- Connolly, H. M., Crary, J. L., McGoon, M. D., Hensrud, D. D., Edwards, B. S., Edwards, W. D., & Schraff, H. V. (1997). Valvular Heart Disease Associated with Fenfluramine–Phentermine. New England Journal of Medicine, 337(24), 1772-1776. doi/full/10.1056/NEJM199712113372414
- WebMD. (2019). Phentermine Oral: Uses, Side Effects, Interactions, Pictures, Warnings & Dosing.
- CardioSmart: American College of Cardiology. (2011, November 21). Phentermine.
- U.S. Food and Drug Administration. (2012). Adipex-P (phentermine hydrochloride) capsules label [Brochure].
- Buchwald, H., Cowan, G. S., & Pories, W. J. (2007). Surgical management of obesity. Philadelphia, PA: Elsevier.
- Lewis, K.H., Fischer, H., Ard, J., Barton, L., Bessesen, D.H., Daley, M.F., Desai, J., Fitzpatrick, S.L., Horberg, M., Koebnick, C., Oshiro, C., Yamamoto, A., Young, D.R. and Arterburn, D.E. (2019), Safety and Effectiveness of Longer-Term Phentermine Use: Clinical Outcomes from an Electronic Health Record Cohort. Obesity, 27: 591-602. https://doi.org/10.1002/oby.22430
- Fourie, A., Julyan, M., Mostert, L., & Du Plessis, J. M. (2023). Potential drug-drug interactions with phentermine among long-term phentermine consumers: A retrospective analysis. South African Medical Journal, 113(8). https://doi.org/10.7196/SAMJ.2023.v113i8.428
- Sendil, S., Gjergjindreaj, M., Lozier, M., & Fernandez, R. (2022). Positive Regadenoson Stress Test in a Patient on Phentermine With Normal Coronaries. Cureus, 14(12), e32138. https://doi.org/10.7759/cureus.32138
- Lewis, K.H., Fischer, H., Ard, J., Barton, L., Bessesen, D.H., Daley, M.F., Desai, J., Fitzpatrick, S.L., Horberg, M., Koebnick, C., Oshiro, C., Yamamoto, A., Young, D.R. and Arterburn, D.E. (2019), Safety and Effectiveness of Longer-Term Phentermine Use: Clinical Outcomes from an Electronic Health Record Cohort. Obesity, 27: 591-602. https://doi.org/10.1002/oby.22430
- Jo, H. S., Wang, S. M., & Kim, J. J. (2019). Recurrent Psychosis after Phentermine Administration in a Young Female: A Case Report. Clinical psychopharmacology and neuroscience : the official scientific journal of the Korean College of Neuropsychopharmacology, 17(1), 130–133. https://doi.org/10.9758/cpn.2019.17.1.130
- Kim KK. Safety of Anti-Obesity Drugs Approved for Long-Term Use. JOMES 2015;24:17-27. https://doi.org/10.7570/kjo.2015.24.1.17
- Jordan, J., Astrup, A., Engeli, S., Narkiewicz, K., Day, W. W., & Finer, N. (2014). Cardiovascular effects of phentermine and topiramate: a new drug combination for the treatment of obesity. Journal of hypertension, 32(6), 1178–1188. https://doi.org/10.1097/HJH.0000000000000145
- Derosa, G., & Maffioli, P. (2012). Anti-obesity drugs: a review about their effects and their safety. Expert opinion on drug safety, 11(3), 459–471. https://doi.org/10.1517/14740338.2012.675326
- Surapaneni, P., Vinales, K. L., Najib, M. Q., & Chaliki, H. P. (2011). Valvular heart disease with the use of fenfluramine-phentermine. Texas Heart Institute journal, 38(5), 581–583.
- Nathan, P.J., O’Neill, B.V., Napolitano, A. and Bullmore, E.T. (2011), Neuropsychiatric Adverse Effects of Centrally Acting Antiobesity Drugs. CNS Neuroscience & Therapeutics, 17: 490-505. https://doi.org/10.1111/j.1755-5949.2010.00172.x
- Kang, J. G., Park, C. Y., Kang, J. H., Park, Y. W., & Park, S. W. (2010). Randomized controlled trial to investigate the effects of a newly developed formulation of phentermine diffuse-controlled release for obesity. Diabetes, obesity & metabolism, 12(10), 876–882. https://doi.org/10.1111/j.1463-1326.2010.01242.x
- Bang, W. D., Kim, J. Y., Yu, H. T., Cho, S. S., Jang, J. Y., Oh, C. M., Joung, B., & Chang, H. J. (2010). Pulmonary hypertension associated with use of phentermine. Yonsei medical journal, 51(6), 971–973. https://doi.org/10.3349/ymj.2010.51.6.
- Loke, Y. K., Derry, S., & Pritchard-Copley, A. (2002). Appetite suppressants and valvular heart disease – a systematic review. BMC clinical pharmacology, 2, 6. https://doi.org/10.1186/1472-6904-2-6
- Ryterska K, Kordek A, Załęska P. Has Menstruation Disappeared? Functional Hypothalamic Amenorrhea—What Is This Story about? Nutrients. 2021; 13(8):2827. https://doi.org/10.3390/nu13082827
- Jones, K. L., Johnson, K. A., Dick, L. M., Felix, R. J., Kao, K. K., & Chambers, C. D. (2002). Pregnancy outcomes after first trimester exposure to phentermine/fenfluramine. Teratology, 65(3), 125–130. https://doi.org/10.1002/tera.10023

